The most common question Ontario clinic owners ask when planning a renovation is: “What should this cost per square foot?” It is also the...
GP & Family Practice Office Renovation in Ontario: Layout, Compliance & Cost Guide (2026)
Dr. Chen had been planning his North York family practice renovation for eighteen months.
The practice had grown from a solo GP to a four-physician group over eight years, and the original 1,800 square foot space — designed for two physicians — was showing every one of those years of overcrowding. Wait times for the single shared procedure room had stretched to 45 minutes on busy mornings. The nurses’ station was a converted broom closet. One exam room still used an analogue blood pressure cuff because there was no wall space for the electronic panel. Dr. Chen had a clear vision: a functional, compliant, modern GP office that could support four physicians operating efficiently. He had a budget of $420,000 and a contractor who had renovated two other medical clinics in York Region. What he did not know — and what his contractor did not tell him — was that one of those previous projects had been a dermatology clinic and the other a chiropractor’s office. Neither had required the CPSO-mandated procedure room specifications, the infection prevention and control standards for primary care settings, or the EMR infrastructure coordination that a GP office required. The project came in at $587,000 and took 11 months. The first CPSO Health Facility Standards inspection found three deficiencies.
This guide covers every technical dimension of GP and family practice office renovation in Ontario — CPSO requirements, exam room specifications, procedure room standards, EMR and technology integration, multi-physician workflow design, AODA compliance, and GTA cost benchmarks for 2026. It is the guide Dr. Chen needed before he signed his renovation contract.
Regulatory Framework: What Governs GP Office Renovation in Ontario
GP and family practice office renovation in Ontario is governed by four regulatory frameworks that operate simultaneously: the College of Physicians and Surgeons of Ontario (CPSO) Health Facility Standards, the Ontario Building Code (OBC), the Accessibility for Ontarians with Disabilities Act (AODA), and Public Health Ontario’s IPAC guidelines for primary care. A contractor who understands only the OBC is missing 75% of the compliance scope for a GP office renovation.
CPSO Health Facility Standards
The CPSO Health Facility Standards apply to physician offices that perform procedures beyond standard physical examination — offices that perform minor surgical procedures, infusion therapy, sedation, or diagnostic imaging require assessment under the Health Facility Standards and may require CPSO inspection before opening. For standard GP offices providing primary care without procedural services, CPSO standards set expectations through the College’s Practice Advisor program and its written guidance on infection prevention, physical examination facilities, and medical record privacy. A GP office that provides minor procedures (punch biopsies, laceration repairs, IUD insertions, joint injections) must ensure that the procedure room meets specific CPSO IPAC standards for surface cleanability, hand hygiene stations, and waste disposal — the same standards that generated three deficiencies in Dr. Chen’s North York renovation.
Public Health Ontario IPAC Guidelines for Primary Care
Public Health Ontario’s IPAC guidance documents for primary care settings establish material standards, hand hygiene infrastructure requirements, and sterilization and disinfection protocols applicable to GP offices. Key IPAC requirements for GP office renovation: hand hygiene sinks must be accessible within the patient zone of every exam room (not outside the room), with hands-free faucet operation specified in procedure rooms; surface materials in exam rooms and procedure rooms must be non-porous and compatible with healthcare-grade disinfectants; and waste disposal facilities must separate sharps (phlebotomy, injection) from non-sharps waste within each clinical room. The IPAC requirements for GP offices are less stringent than those for surgical suites or dental offices but are significantly more stringent than those for general commercial office environments.
AODA Design of Public Spaces Standard
GP offices serving the general population must be fully accessible under AODA O. Reg. 413/12 DOPS. Specific requirements: accessible parking within 30 metres of the accessible entrance, accessible entry with a power door operator (required for all new construction and major renovations under Ontario Building Code Part 3), reception counter with an accessible section at maximum 860mm height with knee clearance, accessible washroom with specific grab bar placement, turning radius, and fixture heights, and an accessible route to all patient-accessed spaces including all exam rooms. A GP office that cannot accommodate a standard powered wheelchair in every exam room with the exam table deployed is non-compliant with AODA — a compliance issue that is expensive to correct if not addressed in the renovation design phase.
GP Office Layout Principles: Designing for Clinical Efficiency

GP office layout is a specialized discipline that differs from general medical office design in three key ways: patient volumes are high (15–30 patients per physician per day), patient acuity is unpredictable (routine physicals and acute presentations mixed in the same day), and workflow involves multiple care team members (physician, nurse, medical administrative assistant) whose paths should not intersect unnecessarily. Three layout principles have the greatest impact on clinical efficiency in GP office design.
The Race-Track Corridor vs. Linear Corridor
Linear corridor layouts — a single hallway with exam rooms on one or both sides — create bottlenecks at reception, force patients to pass each other in the corridor (privacy and infection control concern), and create dead-end circulation paths that reduce staff efficiency. Race-track corridor layouts — a loop corridor with exam rooms around the perimeter and a central work core (nurses’ station, shared equipment, EMR workstations) — allow multi-directional patient flow, give nursing staff central visibility to all room doors, and reduce hallway travel distances between exam rooms. For GP offices with four or more physicians, race-track circulation adds 8–12% to construction costs (due to additional corridor square footage) but reduces nurse travel time by an estimated 25–35 minutes per day per nurse — a productivity return that pays back the construction premium within the first year of operation.
Exam Room Sizing for Ontario GP Offices
CPSO guidance and OBC accessibility requirements together define the practical minimum exam room size for a GP office in Ontario. A room that accommodates an exam table, a physician’s workstation, a nurse’s position, and a patient companion chair — while providing a 1,500mm turning radius for wheelchair access (AODA requirement) — requires a minimum of 10’×12′ (approximately 11 square metres) clear floor area. Rooms smaller than 10’×10′ cannot meet the AODA turning radius requirement with standard exam table dimensions and are non-compliant for new construction. The practical GP exam room specification in GTA renovations is 10’×12′ to 12’×14′ depending on the procedures performed in the room — rooms used for pelvic examinations require an additional privacy curtain zone and often a separate hand washing sink position, adding 2–4 square feet to the functional requirement. Procedure rooms for minor surgical procedures require a minimum of 12’×14′ with a dedicated scrub sink (hands-free) and room for equipment and sterile field maintenance.
Nurses’ Station and Central Work Core
The nurses’ station in a multi-physician GP office is the operational hub — it is where patient vitals are recorded, medications are prepared, forms are completed, and care coordination happens. A nurses’ station designed for 2–3 nurses serving 4 physicians requires: 6–8 linear feet of counter space with EMR workstations at ergonomic height (680–720mm for seated work), dedicated medication preparation area separated from general chart documentation area, direct sightlines to all exam room doors (visual monitoring without leaving the station), and proximity to both the procedure room and the shared equipment storage. GP offices that position the nurses’ station at reception rather than at the clinical core typically find that nursing staff spend 30–40% of their time walking between reception and the clinical zone — time that is not recovered as patient care time.
Exam Room Technical Requirements
Every GP exam room must be equipped to the same standard — inconsistency between rooms creates workflow delays when a physician needs to use a room that lacks a specific piece of equipment or infrastructure. Standard exam room infrastructure in a 2026 Ontario GP office includes the following.
Hand Hygiene Infrastructure
Every exam room requires a dedicated hand hygiene sink, located within the patient care zone (inside the room) and accessible without leaving the clinical area. IPAC guidance specifies: hands-free operation (sensor or wrist-lever faucet), liquid soap dispenser at the sink (not bar soap), paper towel dispenser within reach of the sink, and sharps container mounted adjacent to the sink (at 32–44 inches height, accessible from standing position). Alcohol-based hand rub (ABHR) dispensers at the room entrance do not substitute for a hand washing sink — both are required in exam rooms under PHO IPAC primary care guidance. In renovations of older GP offices where sink installation in every exam room would require significant plumbing rough-in costs, an IPAC consultant can assess whether ABHR-only rooms are permissible for specific examination types — but new construction must include a sink in every exam room.
EMR Workstation and Technology Infrastructure
Modern GP exam room design integrates EMR (Electronic Medical Record) workstations into the room layout rather than treating them as an afterthought. EMR workstations in exam rooms require: a dedicated power circuit at the workstation location (separate from clinical equipment circuits), Cat6 ethernet rough-in to each exam room (Wi-Fi is an acceptable supplement but wired connection is required for clinical reliability), and monitor mounting that allows the physician to maintain eye contact with the patient while referencing the EMR — typically an articulating arm mount that allows the monitor to swivel between physician-facing and patient-facing positions. Practices using integrated clinical documentation systems (including diagnostic equipment auto-population) require USB-A and USB-C ports at the workstation for peripheral device connectivity. Specifying this infrastructure at rough-in stage costs $300–$600 per room in materials; adding it after walls are closed costs $1,200–$3,500 per room.
Medical Gas and Suction Rough-In
Standard GP exam rooms used for physical examination do not require medical gas or suction rough-in. However, procedure rooms in GP offices that perform minor procedures (suture repair, biopsy, joint injection, infusion therapy) require: medical-grade suction (a separate piped system or portable suction with IPAC-compliant cleaning protocol), and in some cases medical oxygen for sedation-adjacent procedures. If a GP practice anticipates adding procedure types in the future, installing rough-in conduit and blocking for medical gas and suction connections at construction time costs $800–$2,400 per connection location — dramatically less than opening walls to add connections post-construction. A Markham family health team practice that installed suction rough-in in its procedure room during a 2023 renovation activated the connection 18 months later when a locum with wound care expertise joined the practice — the $1,600 rough-in investment avoided a $9,000 wall-opening job.
Procedure Room Standards for GP Offices
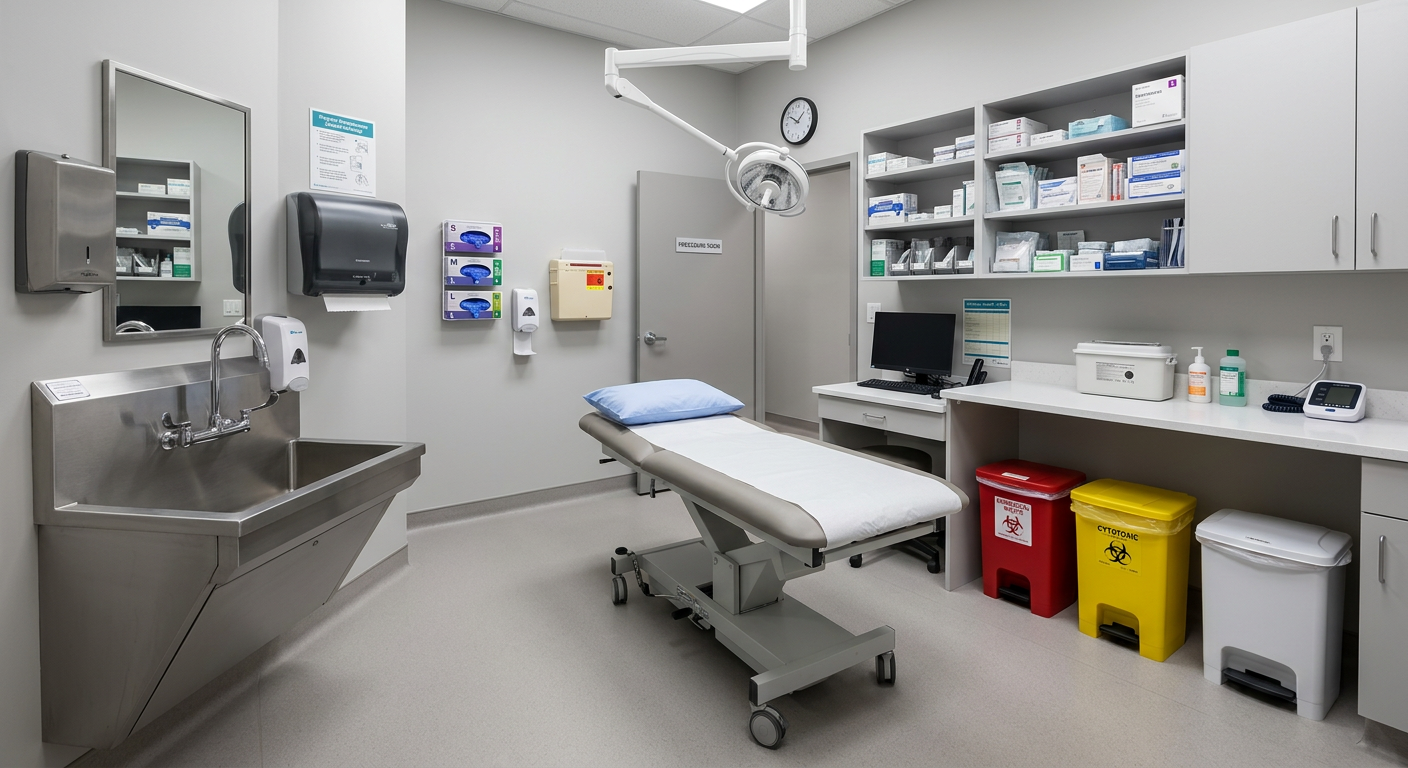
A GP procedure room is the highest-specification space in a primary care office — it must meet CPSO IPAC standards for minor surgical procedures while maintaining the flexibility to accommodate a wide range of non-surgical procedures (phlebotomy, infusion, ECG monitoring, spirometry, audiometry screening). The procedure room specification that satisfies all of these requirements is as follows.
| Element | Specification | Notes |
|---|---|---|
| Room size | Minimum 12’×14′ (180 sq ft) clear floor | Smaller rooms cannot meet CPSO instrument table setup + sterile field requirements |
| Flooring | Seamless: welded-seam sheet vinyl or poured epoxy with integral coved base | Grouted tile non-compliant for IPAC under PHO guidance |
| Wall finish | Semi-gloss alkyd paint or FRP panels in splash zones | Standard latex paint insufficient for repeated disinfection |
| Countertop | Solid surface (Corian, HI-MACS) with undermount sink | No laminate countertops — delamination risk at sink cutout |
| Scrub sink | Deep stainless scrub sink, wrist-lever or sensor faucet | Separate from general hand wash sink; required for surgical procedures |
| Lighting | Exam light (mobile or ceiling-mounted) + 3,500K ambient minimum 500 lux | Mobile exam lights require floor space allocation in room design |
| HVAC | Minimum 4 ACH total, no recirculated air in surgical procedure rooms | Standard GP procedure rooms do not require positive pressure |
| Medical gas | Suction rough-in minimum; oxygen rough-in if sedation possible | Future-proof even if not immediately activated |
| Electrical | 4× duplex outlets, dedicated 20A circuit for procedure equipment | ESA medical-grade outlet requirements apply |
| Privacy | Full-height walls, door with lock, acoustic privacy (STC-40 minimum) | PHIPA patient confidentiality requirement |
Multi-Physician Practice: Scaling Layout for 2 to 6 Physicians
GP office layout requirements change significantly as the number of physicians increases. Understanding these scaling requirements before committing to a space size prevents the overcrowding problem that forced Dr. Chen’s North York renovation.
| Physician Count | Minimum Square Footage | Exam Rooms Required | Support Spaces | Typical GTA Build Cost |
|---|---|---|---|---|
| 1 physician (solo) | 900–1,200 sq ft | 2 exam rooms | Reception, 1 washroom, nurse station | $180,000–$280,000 |
| 2 physicians | 1,400–1,800 sq ft | 3–4 exam rooms | Reception, 2 washrooms, procedure room, nurse station | $260,000–$380,000 |
| 3–4 physicians | 2,200–3,000 sq ft | 6–8 exam rooms | Reception, 2–3 washrooms, procedure room, dictation area | $420,000–$640,000 |
| 5–6 physicians (FHT) | 3,500–5,000 sq ft | 10–14 exam rooms | Full reception, 3–4 washrooms, 1–2 procedure rooms, MDT room | $680,000–$1,200,000 |
Three Most Expensive GP Office Renovation Mistakes
Mistake 1: Undersizing Exam Rooms Below AODA Minimum
The most common costly mistake in GP office renovation is building exam rooms that cannot accommodate a wheelchair patient and a companion simultaneously — which means rooms smaller than 10’×12′ (3.05m×3.66m) for standard exam tables. This mistake is made by both inexperienced architects and by clinicians who accept smaller rooms to increase the count of rooms in a fixed square footage. The remediation — demolishing and rebuilding non-compliant exam room walls — costs $18,000–$45,000 per room pair in a typical GTA renovation. A Scarborough family health team practice built seven exam rooms in a 2,600 square foot fit-out, with room dimensions of 9’×10′ — too small for AODA compliance. Remediation rebuilt four of the seven rooms to 10’×12′ by eliminating one room from the count, at a cost of $67,000. The practice now operates six exam rooms rather than seven — exactly the count it would have had if the original layout had been designed to code.
Mistake 2: Inadequate Plumbing Rough-In Leads to Post-Construction Sink Additions
IPAC requirements mandate a hand hygiene sink in every exam room. GP office renovations that specify a central hand washing station in the corridor — expecting physicians to wash hands between rooms — are non-compliant with PHO IPAC primary care guidance and will be cited in any inspection that references the guidance. Adding hand washing sinks post-construction to existing exam rooms requires: opening the wall to add plumbing rough-in (or trenching the concrete floor if plumbing must be relocated from below), patching and repainting, and potentially rerouting electrical work that conflicts with the new plumbing. Average cost of post-construction exam room sink addition: $4,500–$9,000 per room. In a four-physician practice with eight exam rooms, that is $36,000–$72,000 in avoidable remediation — far exceeding the cost of proper rough-in at construction time.
Mistake 3: Failing to Separate Clean and Dirty Utility Functions
CPSO IPAC standards for GP offices require separation of clean utility functions (medication preparation, clean supply storage, sterile equipment storage) from dirty utility functions (instrument cleaning, waste disposal, soiled linen holding). In many GP office renovations, a single “utility room” attempts to serve both functions — a design that is non-compliant with IPAC guidance and creates infection control risk. The minimum compliant approach: a clean utility room (or designated clean zone within the nurses’ station) separated from a dirty utility room (containing a deep service sink, autoclave, sharps waste, and soiled material holding). In small GP offices with limited square footage, a single utility room with a full-height partition and a one-way door between the clean and dirty zones is an acceptable alternative — but must be explicitly designed with this separation in mind. An Oshawa family practice added this partition retroactively at a cost of $12,000 after an IPAC assessment identified the single-utility-room design as non-compliant.
GP Office Renovation Cost Breakdown by Scope
| Scope Item | Cost Per Unit | Notes |
|---|---|---|
| Exam room (complete fit-out) | $28,000–$55,000 per room | Sink, flooring, walls, lighting, EMR rough-in |
| Procedure room (CPSO-compliant) | $55,000–$120,000 | Includes scrub sink, specialized HVAC, medical gas rough-in |
| Reception and waiting area | $35,000–$90,000 | AODA counter, accessible seating, reception glazing |
| Nurses’ station (central core) | $22,000–$45,000 | Custom millwork, EMR workstations, medication prep area |
| Clean/dirty utility rooms | $18,000–$40,000 combined | Autoclave, service sink, storage |
| Corridor and common areas | $60–$120 per sq ft | Flooring, lighting, signage, accessible washroom |
| HVAC upgrade (per exam room) | $3,500–$8,000 | Individual VAV zones per exam room for privacy and comfort |
| EMR and technology infrastructure | $2,500–$6,000 per room | Cat6, power, monitor mounts, peripheral ports |
GP Office Renovation Compliance Checklist
- All exam rooms minimum 10’×12′ with AODA 1,500mm turning radius maintained with exam table deployed
- Hand hygiene sink inside every exam room (not corridor) with hands-free faucet
- ABHR dispenser at every exam room entrance in addition to sink
- Seamless flooring (welded sheet vinyl or poured epoxy) in procedure room
- Non-porous, disinfectant-compatible flooring in all exam rooms
- Solid surface countertops in procedure room (no laminate)
- Clean utility zone separated from dirty utility zone (physical or partition separation)
- Autoclave in dirty utility room with CPSO sterilization monitoring protocols in place
- Sharps container mounting in every exam room and procedure room (IPAC standard height)
- Procedure room minimum 12’×14′ with dedicated scrub sink and 4+ ACH HVAC
- CPSO IPAC-compliant waste disposal in procedure room (biohazardous + sharps + general)
- AODA-compliant reception counter (860mm max, knee clearance section)
- AODA accessible washroom (turning radius, grab bars, accessible fixtures)
- Power-operated entry door (new construction/major renovation OBC requirement)
- All exam room doors minimum 920mm clear width (AODA passage width)
- Patient privacy acoustic separation between exam rooms (minimum STC-40 partition)
- PHIPA-compliant reception design (reception conversations inaudible in waiting area)
- EMR workstation rough-in (Cat6, power, monitor mount) in every exam room
- Adequate lighting in exam rooms (minimum 300 lux ambient, exam light provision)
- Building permit obtained before any construction begins
5-Phase Implementation Roadmap for GP Office Renovation
Phase 1: Clinical Requirements and Space Planning (Weeks 1–3)
Document the clinical workflows the renovated space must support: physician count, patient volume targets, procedure types performed in-office, nursing staff count, and technology systems in use (EMR platform, diagnostic equipment). Engage an architect or healthcare interior designer with Ontario GP office experience — not a general commercial architect — to conduct a programming session that translates clinical requirements into spatial requirements (room counts, dimensions, adjacencies). Commission an IPAC consultant review concurrent with architectural programming: IPAC requirements drive specific spatial features (sink locations, utility room configuration, procedure room specifications) that must be established before layout is locked.
Phase 2: Design Development and Permit Application (Weeks 3–10)
Architect produces construction drawings with full AODA accessibility documentation, IPAC compliance notes, and mechanical/electrical/plumbing drawings coordinated with the IPAC and technology requirements identified in Phase 1. Building permit application submitted: typical GTA review times range from 4 weeks (Richmond Hill, Newmarket) to 8–10 weeks (City of Toronto). If the practice performs procedures requiring CPSO registration or assessment, initiate CPSO notification concurrently. Contractor tender should begin 4–6 weeks after permit application, with bidders required to demonstrate healthcare renovation experience — ask specifically for references from GP offices that have passed CPSO assessment or IPAC inspection.
Phase 3: Rough-In and Framing (Weeks 10–16)
Plumbing rough-in for exam room sinks is the most critical rough-in milestone — verify every sink location before walls are framed. IPAC review of framing drawings before wall boarding begins. Electrical rough-in including EMR workstation circuits and medical equipment circuits. HVAC rough-in with individual zone dampers per exam room. Medical gas rough-in conduit (even if connections are not immediately activated). Review of all utility room placements relative to patient circulation paths — dirty utility should not be visible from patient areas or accessed through patient corridors.
Phase 4: Fit-Out and Technology Integration (Weeks 16–22)
Millwork installation: exam room cabinetry (overhead and base), nurses’ station millwork, reception counter. Flooring installation starting with procedure room (highest specification), then exam rooms, then corridors and common areas. IT infrastructure: Cat6 termination, wall plate installation, EMR system connectivity testing. Medical equipment installation: exam tables, EMR monitor mounts, diagnostic equipment. AODA compliance verification: measure all counter heights, turning radii, door clearances, and grab bar placements against specification before walls are closed around accessible washroom fixtures. HVAC commissioning: verify individual zone damper operation and airflow balancing in each exam room.
Phase 5: Inspection, Commissioning, and Opening (Weeks 22–26)
Final building inspection for OBC compliance — request the inspection 2–3 weeks before targeted opening date to allow time for any minor deficiencies to be corrected without delaying opening. IPAC final walk-through by IPAC consultant or qualified infection control professional — document all IPAC-relevant features in writing as evidence of due diligence. Staff orientation to IPAC protocols specific to the renovated space (hand hygiene station locations, clean/dirty utility workflows, sharps disposal). Patient communication regarding clinic reopening after renovation — coordinate with your EMR administrator to notify patients of any scheduling changes during construction closure. If CPSO notification is required for your procedure scope, confirm receipt of acknowledgment before performing any regulated procedures in the new space.
GTA City-by-City: Permit Timelines for GP Office Renovation
| Municipality | Permit Review (weeks) | Pre-Application Consultation | Notes |
|---|---|---|---|
| Toronto | 8–12 | Available (book 2–3 weeks ahead) | Highest volume; complex projects may take 14+ weeks |
| Mississauga | 6–9 | Available | Digital submission process; faster than Toronto for small-medium scope |
| Brampton | 6–10 | Limited | Growing clinic market; permit reviewers may have less healthcare experience |
| Markham | 5–7 | Available | York Region coordinated review; efficient for medical occupancies |
| Richmond Hill | 4–7 | Available | Consistent reviewer experience with medical clinics |
| Vaughan | 5–8 | Limited | York Region permit; growing suburban medical market |
| Newmarket/Aurora | 3–5 | Available | Fastest permit turnaround in GTA for GP clinic scope |
PHIPA Privacy Design in GP Office Renovation

The Personal Health Information Protection Act (PHIPA) creates design obligations for GP offices that are rarely addressed by contractors without specific healthcare renovation experience. PHIPA requires that personal health information be protected from unauthorized access and inadvertent disclosure — requirements that translate directly into physical design decisions in the clinic environment.
Reception Desk Acoustic and Visual Privacy
At the reception desk, patients routinely share their name, health card number, reason for visit, and appointment history — all personal health information under PHIPA. Reception desk designs that face the waiting room directly, with low counter heights that allow waiting patients to hear reception conversations, are structurally non-compliant with the spirit of PHIPA’s privacy obligation. Design solutions: reception counter positioned at 90 degrees to the waiting room (patients approach from the side rather than from across the room), acoustic baffling at the reception desk (overhead ceiling baffles that absorb sound before it propagates into the waiting area), and electronic check-in kiosks that allow patients to check in without verbal communication. The electronic kiosk option is increasingly common in GTA GP offices and eliminates the reception privacy problem while reducing administrative workload. Kiosk rough-in (power outlet and network port at kiosk height) should be specified at construction time: $300–$600 per kiosk location.
Exam Room Acoustic Privacy (PHIPA Requirement)
PHIPA requires that patient health information shared during clinical consultations cannot be overheard by other patients. Standard GP exam room partitions using single-stud framing with standard gypsum board achieve STC-35 to STC-40 — adequate to muffle loud conversation but insufficient to prevent intelligible speech transmission between adjacent rooms at normal conversation volumes. PHIPA compliance for exam room acoustic privacy requires STC-45 minimum partition construction between exam rooms: double-stud or staggered-stud framing with acoustic batt insulation, with all penetrations (electrical boxes, conduit) acoustically sealed. The cost delta between standard STC-35 partitions and STC-45 partitions is approximately $12–$18 per square foot of partition — a $600–$900 difference per exam room partition in a typical 10’×12′ room. The legal and reputational risk of a PHIPA complaint alleging patient privacy breach through inadequate sound isolation far exceeds this incremental construction cost.
EMR Workstation Screen Privacy
EMR screens in exam rooms that are visible from the doorway — particularly in rooms where the door is frequently left open during nursing workflows — expose patient health information to corridor passersby. PHIPA-compliant exam room design positions the physician’s EMR workstation so that the screen faces away from the door (toward an interior wall or corner), or uses a monitor privacy filter that limits the viewing angle. In clinics using articulating monitor arms that allow screen sharing with patients, the articulation path should be designed so that the patient-facing position does not expose the screen to the corridor. This design detail costs nothing if addressed in the room layout design phase; it requires monitor relocation or expensive millwork modification if discovered after construction is complete.
Choosing the Right Contractor for Your GP Office Renovation

The Dr. Chen case study that opens this guide illustrates the core problem with GP office contractor selection: a contractor can have genuine medical clinic experience — even successful projects in that category — without having the specific experience relevant to your renovation scope. Two questions separate qualified GP office renovation contractors from general medical contractors who will discover the gaps in their knowledge during your project.
The Five Qualification Questions for GP Office Contractors
Question 1: “Have you completed a GP or family medicine clinic renovation where the practice performs in-office procedures, and did the renovation include a CPSO-compliant procedure room?” A contractor who has completed dental or chiropractic clinic renovations has not demonstrated GP-specific IPAC knowledge. Ask for the specific project and the physician’s name — you can call the physician to verify.
Question 2: “How do you specify hand washing sink installation in exam rooms, and what is your standard approach to exam room plumbing rough-in coordination?” A qualified contractor immediately describes coordinating sink locations with IPAC requirements and specifying hands-free faucets. A contractor who asks “how many sinks do you need?” has not thought about the IPAC standard that drives the answer.
Question 3: “What partition construction standard do you use between exam rooms for acoustic privacy, and why?” A qualified contractor specifies STC-45 minimum and explains PHIPA acoustic privacy obligations. A general contractor typically answers with the minimum OBC requirement, which does not address PHIPA compliance.
Question 4: “What is your process for coordinating with the practice’s EMR and technology vendor during rough-in?” A qualified contractor has a standard technology coordination process. A general contractor will either have never thought about this or will suggest the practice handle it separately — creating the conditions for the $1,200–$3,500 post-construction retrofit described above.
Question 5: “Have you had a stop-work order or a compliance deficiency citation on any medical clinic project, and what happened?” A forthright answer with explanation is acceptable. Evasion is a red flag. No healthcare-experienced contractor has an unblemished record — what matters is how they managed the issue and what they learned.
A contractor who answers all five questions specifically, with project names, physician references, and technical detail, is a qualified GP office renovation contractor. A contractor who answers three of five specifically, with references, is a borderline candidate who should be evaluated on their references’ feedback. A contractor who cannot answer the first two questions specifically should not receive a bid invitation for a GP office renovation, regardless of their pricing.
Financial Planning for Your GP Office Renovation in Ontario
GP office renovation is among the largest single capital expenditures most family physicians will make outside of purchasing a home or clinic property. Financial planning for the renovation — beyond simply obtaining the lowest contractor quote — involves understanding financing structures available to healthcare professionals, tax treatment of renovation costs, and the revenue impact of clinical closure during construction.
Financing Options for Ontario GP Office Renovations
Healthcare professionals have access to specialized financing products not available to general commercial borrowers. Medical practice loans from major Canadian banks (BMO Healthcare Practice Banking, RBC Healthcare, Scotiabank Medical Professional Program) offer higher loan-to-value ratios, longer amortization periods, and lower rates than standard commercial loans for qualified physicians. Typical terms for a GP office renovation loan in 2026: prime + 0.25% to prime + 0.75%, amortization up to 15 years, loan amounts up to $1,500,000 for established practices. The practice’s OHIP billing history is the primary credit assessment input — practices with three or more years of consistent OHIP billing history and a plan that demonstrates patient volume retention through the renovation period are routinely approved. Leasehold improvement financing — where the lender takes a security interest in the leasehold improvements — is the most common structure; it does not require property collateral, making it accessible to practices in leased premises.
Revenue Impact Calculation and Break-Even Analysis
A four-physician GP practice billing $320,000 annually in OHIP per physician loses approximately $6,150 in weekly revenue during a full clinical closure. A 10-week closure for a complete renovation costs approximately $61,500 in lost OHIP billings — a cost that does not appear in the renovation budget but is real. Including this cost in the renovation decision and financing model produces a more accurate total project cost. Practices that phase renovation to maintain partial clinical operation during construction (see Phase 3 above) reduce this revenue loss by 40–60%, though phased construction adds 20–35% to the project timeline and 8–15% to direct construction costs due to phasing complexity. The break-even analysis for phased versus closed renovation typically favours closed renovation for projects longer than 8 weeks at full replacement scale — but requires practice-specific calculation based on per-physician billing rates and the cost premium of phased construction.
Frequently Asked Questions: GP Office Renovation in Ontario
Does a GP office renovation require CPSO approval?
A standard GP office providing primary care (physical examinations, diagnosis, prescription management, routine immunization) does not require formal CPSO approval of the facility before opening. GP offices that add procedural services — minor surgery, conscious sedation, infusion therapy, or diagnostic imaging — must notify CPSO and may be subject to a Health Facility Standards inspection before performing those procedures. The best practice is to consult CPSO’s Practice Advisory Service before beginning a major renovation if the scope of services performed in the new office will expand beyond standard primary care. CPSO advisors can confirm whether CPSO notification is required for your specific practice scope without charge.
What is the cost of a single exam room fit-out in Ontario?
A complete exam room fit-out in Ontario — including flooring, plumbing for the exam room sink, IPAC-compliant wall finishes, cabinetry, exam light provision, EMR workstation rough-in, and HVAC zone — costs $28,000–$55,000 per room in 2026 GTA pricing. The range reflects: the flooring specification (poured epoxy at the high end, welded sheet vinyl at the low end), the millwork scope (custom built-in cabinetry versus semi-custom), and the plumbing complexity (existing rough-in nearby lowers cost; new branch off the main stack raises it). A four-physician practice with eight exam rooms should budget $224,000–$440,000 for exam rooms alone, before adding procedure room, reception, nursing station, utility rooms, and common areas.
Can a GP office stay open during renovation?
Yes, GP offices can often operate during renovation if the construction is phased so that clinical areas remain accessible while non-clinical areas are under construction. Phased renovation requires careful IPAC management: construction zones must be sealed with dust barriers, negative pressure is required in construction zones adjacent to active clinical spaces, and HVAC zones must be isolatable between construction and clinical areas. The most common phasing approach is to operate from a portion of the existing space (or temporary space) while the renovation proceeds in the remainder, then migrate in phases. This approach typically adds 20–35% to project duration but eliminates the revenue loss of complete clinical closure. An IPAC consultant should review and approve the phasing plan before construction begins.
What EMR system infrastructure should be roughed-in during renovation?
Every exam room and workstation should receive: Cat6 ethernet rough-in (minimum two ports per workstation location), power circuits with at least two duplex outlets on a dedicated 20A circuit for the workstation, and conduit or cable management system for monitor mounting (either a ceiling-mounted arm or a wall-mounted articulating arm). For practices using voice recognition or AI documentation tools, a USB hub location near the physician’s workstation accommodates the microphone connection. For practices using integrated diagnostic equipment (spirometry, audiometry, ECG systems that auto-populate the EMR), additional USB ports and equipment mounting provisions should be specified at rough-in stage. Consult your EMR vendor before finalizing the technology rough-in specification — vendor representatives will provide a standard exam room technology requirement document at no charge for practices actively planning a renovation.
How many exam rooms does a GP need?
The industry standard for exam room allocation in a GP practice is 2.5 exam rooms per physician — a ratio that accounts for patient preparation time (a patient in one room being assessed by the nurse), active physician time (the physician with a patient in a second room), and a buffer room for overflow or special procedures. A solo GP needs 2 rooms minimum; 3 is optimal. A two-physician practice needs 4–5 rooms. A four-physician practice needs 8–10 rooms. Practices that build only 1.5 rooms per physician — a common budget-reduction decision — consistently find that room availability becomes the binding constraint on patient volume within the first year. Building an additional exam room during the original renovation is far less expensive than adding one after construction is complete: the marginal cost of an additional exam room during construction is $28,000–$40,000 versus $55,000–$90,000 to add a room post-construction by modifying an existing non-clinical space.
What is the difference between a family health team and a standard GP office renovation?
A Family Health Team (FHT) is an Ontario primary care model that includes nurse practitioners, social workers, dietitians, and other allied health professionals alongside family physicians. FHT renovations require: private office space for each non-physician clinician (for individual consultations), a multidisciplinary team meeting room (for case conferences and team meetings), and a larger nursing station to accommodate the expanded care team. FHT facilities typically also include group education rooms for chronic disease management programs — a space type not present in standard GP offices. FHT renovation costs are significantly higher than standard GP office costs: a typical 4-physician FHT with allied health staff occupies 4,000–6,000 square feet and costs $800,000–$1,500,000 all-in for a complete fit-out from shell space.
Do I need AODA compliance in an existing GP office?
If you are renovating an existing GP office — particularly a space that has been a clinic for many years — AODA compliance requirements are triggered by the scope of the renovation. Under the Ontario Building Code, any renovation permit that constitutes more than 50% of the building’s value triggers full accessibility compliance for the altered portions. Even below that threshold, AODA’s accessibility requirements apply to newly constructed or significantly altered areas. As a practical matter: any GP office renovation that moves walls, replaces reception counters, or modifies bathrooms should achieve full AODA DOPS compliance in those elements. The reputational and legal risk of operating a physician office with documented accessibility deficiencies is disproportionate to the cost of achieving compliance during a renovation.