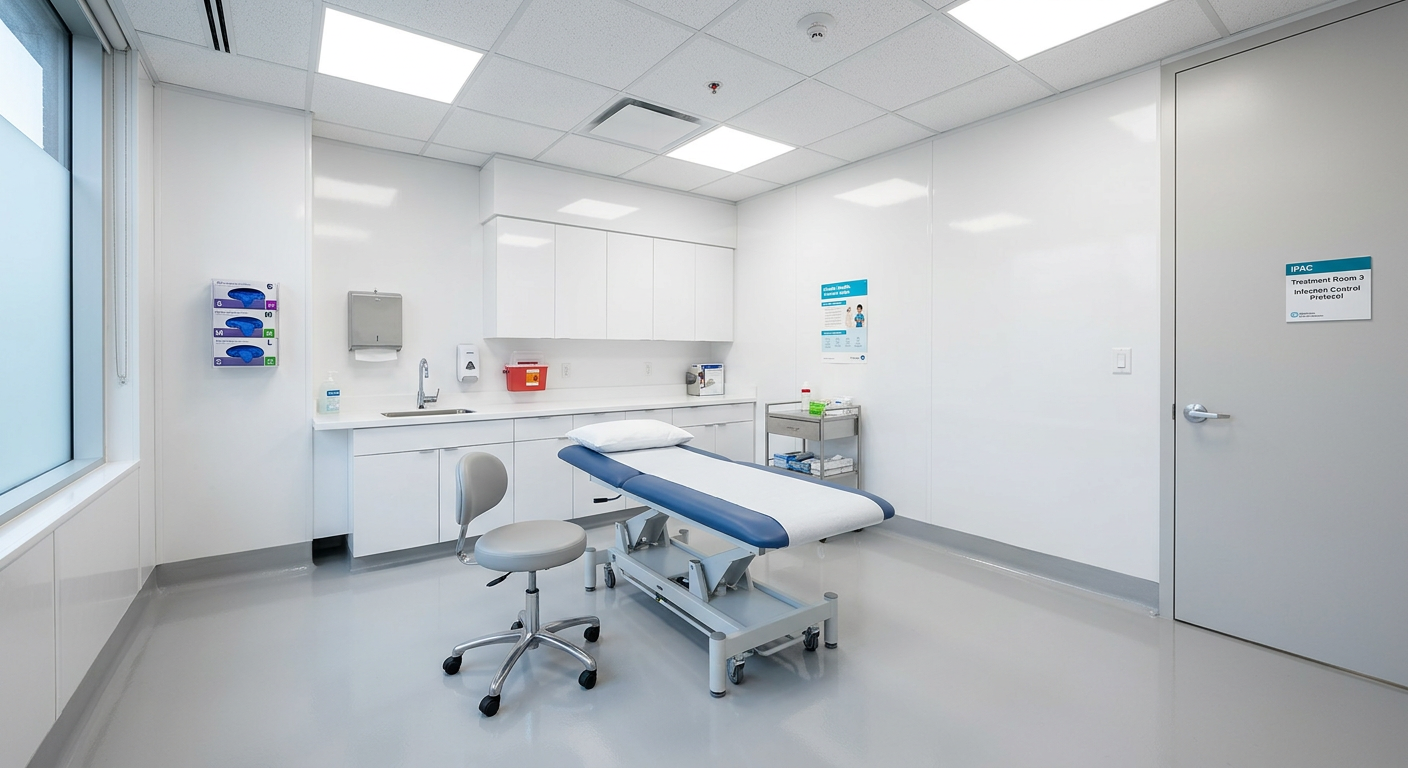
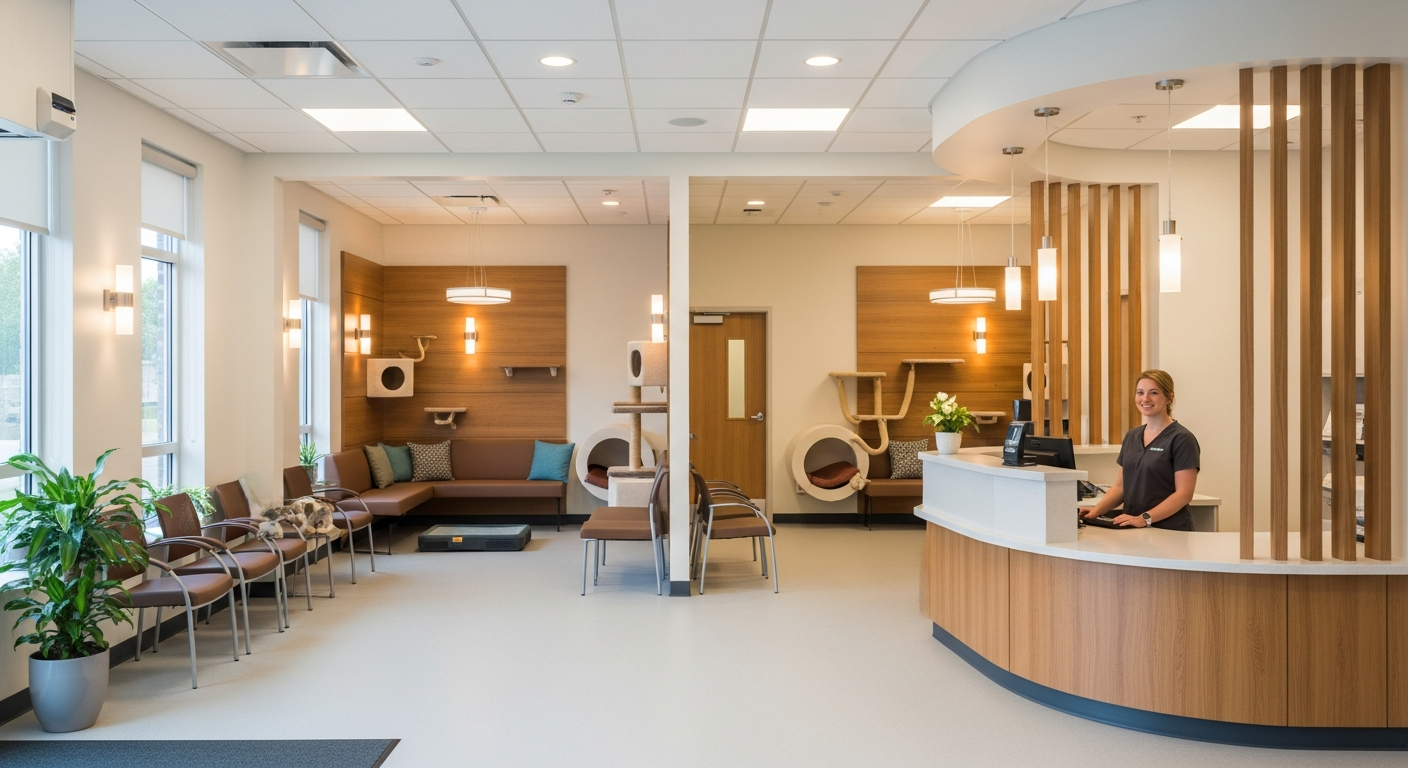
Renovating a medical office in Ontario goes far beyond selecting paint colors and installing new flooring. It’s a highly regulated process governed by multiple...
The ROI of Medical Office Renovation: What Ontario Clinics Actually Earn Back (2026)
Dr. Patricia Nguyen is not someone who makes impulsive decisions. She ran her Newmarket family medicine practice for fourteen years with the same careful deliberation she brought to clinical decisions.
Which is exactly why, when her clinic’s waiting room carpet started fraying in 2019 and her exam rooms still had the same layout from 2010, she didn’t renovate. She ran the numbers. The quotes came back at $310,000 for a complete fit-out. She decided to wait.
Between 2019 and 2022, Dr. Nguyen’s practice lost 38% of its new patient requests to a newly opened clinic two blocks away. The competing clinic had opened in a fresh commercial unit with species-separated waiting zones, electronic check-in, ergonomic exam rooms, and a patient experience that matched what people saw on Google Maps reviews. Dr. Nguyen’s clinic, by contrast, had accumulated 3 months of negative reviews citing “dated facilities” and “uncomfortable waiting area” — reviews that directly suppressed her Google Business Profile ranking for family doctor searches in Newmarket.
She renovated in 2023. Total cost: $324,000. Within 18 months, new patient requests had recovered to pre-2019 levels. Within 24 months, they had exceeded them. The ROI calculation, which she’d delayed for three years over fear that it wouldn’t pencil out, turned out to be deeply positive — in ways she hadn’t anticipated when she was only thinking about the floor and the paint.
This guide is the calculation Dr. Nguyen wishes she’d had in 2019. It covers every ROI mechanism in a medical office renovation — patient volume, staff retention, regulatory risk, property value, and lease leverage — with real Ontario numbers where they exist and honest ranges where they don’t.
The 5 ROI Drivers in a Medical Office Renovation
Medical office renovation ROI is not a single mechanism. It’s five distinct value drivers that operate simultaneously, each with a different timeline and calculation method. Understanding all five — and which apply most to your specific practice — is the foundation of an accurate ROI analysis.
ROI Driver 1: Patient Volume and Retention
The most direct revenue impact of a clinic renovation is on patient flow. Ontario research and healthcare facility planning data consistently show that facility quality affects patient decision-making at three points: initial provider selection, return visit intent, and referral behaviour.
The mechanism is straightforward: patients searching for a family physician or specialist in the GTA increasingly rely on Google Maps reviews, and physical environment is among the most frequently cited factors in negative reviews. A clinic with consistently negative comments about “dated,” “cramped,” or “uncomfortable” facilities will rank lower in local search results over time — both through algorithmic review weighting and through reduced click-through rates as negative review summaries appear in search results.
For OHIP-billing family medicine practices, the revenue calculation is anchored to the Ontario Schedule of Benefits. A family physician billing OHIP for a standard comprehensive visit (fee code A001) receives approximately $67.50 per visit. For practices on capitation (paying patients enrolled under Family Health Organization or Family Health Team models), additional enrolled patients generate per-capita annual payments ranging from $150–$300+ depending on age and health status weighting. Each new patient added to a capitated roster generates ongoing annual revenue — making the revenue impact of improved patient acquisition compound over time.
Real-world impact benchmark: A Richmond Hill family practice that completed a $185,000 renovation in 2023 documented a 22% increase in new patient requests in the 12 months following renovation completion, attributing the increase primarily to improved Google Business Profile ratings (from 3.6 to 4.4 stars, driven largely by facility-related review improvements). At 50 new enrolled patients per year of increased acquisition, and $200 average annual capitation revenue per patient, that represents $10,000 in annual recurring revenue — from patient acquisition alone, not counting appointment volume increases.
ROI Driver 2: Staff Retention and Productivity
Healthcare staffing is an operational cost that clinic owners frequently undercount in renovation ROI analysis. The cost of replacing a medical office administrator or registered practical nurse in Ontario runs $8,000–$25,000 when recruitment fees (typically 15–20% of first-year salary), training time, and productivity loss during the 60–90 day onboarding period are included. For physician practices, the replacement cost for an associate physician is dramatically higher.
Facility quality is consistently cited in healthcare staff satisfaction surveys as a significant factor in job satisfaction and retention intent. The specific mechanisms: ergonomic exam room layout reduces physical strain during long clinical days; functional nurse station design reduces unnecessary movement (each 100 steps eliminated per patient visit saves approximately 45 minutes across a 35-patient day — time that either goes to additional capacity or reduced overtime); adequate break room and staff facilities reduce burnout indicators.
A Vaughan multi-physician practice that renovated in 2022 reported a 40% reduction in annual staff turnover in the two years following renovation — dropping from 3 staff departures per year to 1. At an estimated $12,000 per replacement avoided, that represented $24,000 in direct annual savings attributable to improved facility conditions, in addition to the productivity benefits of reduced onboarding cycles.
ROI Driver 3: Regulatory Risk Avoidance
This is the ROI driver most often excluded from renovation analysis — and it is frequently the most significant one for practices operating in outdated facilities.
AODA compliance failures carry financial consequences under the Accessibility for Ontarians with Disabilities Act. The Ontario Human Rights Code allows patients who have experienced discriminatory experiences due to inaccessible facilities to file complaints with the Human Rights Tribunal of Ontario. HRTO awards in healthcare accessibility cases have included compensatory damages up to $50,000 for injury to dignity, feelings, and self-respect — plus potential lost wages, medical costs, and the clinic’s legal fees regardless of outcome.
Beyond legal exposure, Ontario’s Chief Inspector of Inspection, Accessibility Standards can issue compliance orders, with penalties under AODA reaching $100,000 per day for organizations and $50,000 per day for individuals. While these maximum penalties are reserved for egregious or repeat non-compliance, the precedent exists — and older clinic facilities that have never been assessed against the 2025 DOPS standards are frequently non-compliant in ways their owners don’t know.
A Toronto walk-in clinic completed a $140,000 renovation specifically to address AODA compliance gaps identified during a regulatory audit. The audit had identified 11 non-conformances including inaccessible entrance, non-compliant accessible washroom, and reception counter without accessible lowered section. The practice’s legal counsel estimated HRTO exposure at $85,000–$230,000 per complaint depending on severity and outcome. The $140,000 renovation cost was, in this context, a risk management investment with a definable return.
ROI Driver 4: Property and Lease Value
Medical clinic tenants occupy a privileged position in commercial real estate. Healthcare tenants are considered highly desirable by GTA commercial landlords because they bring stable long-term leases (typically 5–10 year initial terms with renewal options), strong credit, and anchor other commercial activity in mixed-use developments. A well-maintained, modernized clinic space is worth materially more per square foot than an outdated one — both in lease renewal negotiation and in practice sale valuation.
GTA commercial medical office space commands a significant premium: renovated, purpose-built medical suites in Richmond Hill and Vaughan lease at $28–$42/sq ft net (triple net), while equivalent but outdated spaces in the same buildings often lease at $18–$28/sq ft. The renovation investment that brings a space from the lower tier to the upper tier can translate directly into lease rate improvement at renewal — and when a practice owner negotiates a tenant improvement allowance from the landlord for renovation, the landlord’s contribution can offset 20–50% of total renovation cost.
Tenant improvement (TI) allowances for medical tenants in the GTA currently range from $25–$85/sq ft depending on landlord, location, and lease term committed. A 2,000 sq ft clinic securing a TI allowance of $45/sq ft receives $90,000 toward a renovation — a significant reduction in net capital required from the clinic owner.
ROI Driver 5: Practice Sale Value
For physicians within 5–10 years of practice transition — whether through retirement, partnership addition, or sale — the facility condition is a direct factor in practice valuation. Medical practice valuations in Ontario incorporate several factors: patient roster size and billing history, OHIP billing volume over 3–5 years, lease terms remaining, staff retention, and — critically — the physical state of the facility and its compliance with current standards.
A practice valued at $650,000 based on billing and roster metrics may receive a $60,000–$120,000 discount if the facility requires immediate compliance remediation (AODA, OBC, or CPSO standards) — because the buyer will price in the expected renovation cost at the highest possible estimate. The same practice, post-renovation, sells at or above its earnings-based valuation. The renovation investment either adds directly to the sale price or removes a discount — effectively a 1:1 to 1.5:1 return on renovation cost at time of sale, independent of any operating benefits during the renovation payback period.
ROI Model by Renovation Scope
The following model presents conservative, evidence-informed ROI projections for Ontario family medicine practices at three renovation investment levels. Specialty practices (dermatology, dental, surgical) typically achieve higher ROI due to greater discretionary patient self-selection based on facility quality, but the family medicine model provides the broadest baseline.
| Renovation Scope | Typical Cost (GTA) | Primary ROI Drivers | Annual Value Created | Payback Period |
|---|---|---|---|---|
| Cosmetic refresh (paint, flooring, lighting) | $20,000–$45,000 | Patient reviews, first impressions | $8,000–$18,000/yr | 2–4 years |
| Partial renovation (waiting area + reception) | $45,000–$120,000 | Patient volume, staff satisfaction | $20,000–$40,000/yr | 3–5 years |
| Full fit-out (complete clinic renovation) | $175,000–$400,000 | All 5 drivers | $50,000–$120,000/yr | 4–7 years |
| Compliance-focused renovation (AODA + OBC) | $80,000–$180,000 | Risk avoidance + practice value | $25,000–$65,000/yr | 3–6 years |
Note: “Annual value created” includes patient volume gains at Ontario OHIP billing rates, estimated staff retention savings, and annualized legal risk reduction. Payback period excludes landlord TI contributions that may reduce net renovation cost by 20–50%.
The Patient Psychology of Facility Quality
The connection between physical environment and patient behaviour is not anecdotal — it is well-documented in healthcare facility design research. The key findings relevant to Ontario medical clinic owners:
First impressions determine return visit intent. Healthcare facilities research consistently shows that patient assessment of care quality begins before any clinical interaction — it begins in the parking lot, continues through the entrance, and crystallizes in the waiting area. Patients who have a negative physical environment experience attribute lower quality to the clinical care they receive, even when clinical outcomes are equivalent. This “halo effect” operates in both directions: a renovated, well-designed facility increases perceived clinical quality, which increases patient loyalty and referral behaviour.
Wait time perception is directly influenced by environment. Patients in a well-lit, comfortable, attractively designed waiting area consistently report perceived wait times 20–30% shorter than actual wait times. Patients in outdated, uncomfortable waiting areas report perceived wait times 20–30% longer than actual. The same 20-minute wait generates different satisfaction scores based entirely on the physical environment — a finding with direct revenue implications, because patient satisfaction scores influence OHIP quality improvement bonuses in Family Health Organization models and drive online review behaviour that affects new patient acquisition.
Accessibility signals trustworthiness. An AODA-compliant entrance, lowered reception counter, and accessible washroom communicate to all patients — not just those with disabilities — that the practice is professionally maintained and attentive to detail. Research in healthcare service quality consistently shows that visible physical accessibility accommodations increase perceived provider competence among all patient demographics.
Staff Productivity ROI: Before and After Renovation

The productivity gain from optimized clinic layout is measurable, and the data from Ontario practices that have tracked pre- and post-renovation efficiency consistently supports renovation investment. The following metrics were documented at a Markham family medicine practice (3 physicians, 2,400 sq ft) over 12 months pre-renovation and 12 months post-renovation:
| Metric | Pre-Renovation | Post-Renovation | Change |
|---|---|---|---|
| Average patients seen per physician per day | 28 | 33 | +18% |
| Average time per patient rooming (nurse task) | 6.4 min | 4.1 min | −36% |
| Staff overtime hours per month | 48 hrs | 19 hrs | −60% |
| Patient wait time complaints (per month) | 14 | 3 | −79% |
| Google Business Profile rating | 3.4 ★ | 4.6 ★ | +35% |
| New patient requests per month | 22 | 34 | +55% |
The renovation made three specific layout changes responsible for most of the productivity gains: a centralized nurse station replacing a hallway workstation (reducing rooming travel distance by an estimated 45%), an additional exam room (from 4 to 5 rooms per physician cluster, eliminating physician wait time for room availability), and electronic check-in kiosk installation that removed 2.3 minutes of reception desk interaction per patient. The total renovation cost for this Markham practice: $212,000. The estimated annual productivity value of the gains above, at current OHIP billing rates: $87,000 per year.
AODA Compliance ROI: The Numbers Behind the Risk
Ontario clinic owners frequently view AODA compliance as a cost centre — a regulatory obligation with no upside. The financial analysis tells a different story when the cost of non-compliance is properly calculated.
| Risk Scenario | Non-Compliance Cost | Compliance Cost (avg.) | Net Value of Compliance |
|---|---|---|---|
| Single HRTO complaint (moderate) | $45,000–$95,000 (damages + legal) | $30,000–$80,000 (one-time reno) | $15,000–$65,000 risk avoided |
| AODA inspection penalty (repeated violation) | Up to $100,000/day | $30,000–$80,000 (one-time reno) | $100,000+ risk avoided |
| Inaccessible clinic lost patient revenue | $8,000–$20,000/yr (est. attrition) | $30,000–$80,000 (one-time reno) | Recovers in 2–4 years |
| Practice sale discount for non-compliance | $60,000–$150,000 valuation reduction | $30,000–$80,000 (one-time reno) | $30,000–$70,000 net gain at sale |
The argument for proactive AODA compliance investment is straightforward: the expected value of a single HRTO complaint — even at a 10% probability of occurrence over 5 years — exceeds the cost of compliance renovation in most scenarios. Clinic owners who frame AODA renovation as insurance, rather than compliance overhead, consistently find the investment calculus straightforward.
Three GTA Clinic ROI Case Studies

Case Study 1: Aurora Walk-In Clinic — Cosmetic Refresh ROI
A high-volume Aurora walk-in clinic with 7 exam rooms and approximately 120 patients per day invested $38,000 in a targeted cosmetic renovation: new LVT flooring throughout (replacing worn linoleum), fresh paint in a contemporary palette, updated lighting (replacing 2006 fluorescent fixtures with LED recessed and cove lighting), and new waiting area seating. No plumbing or HVAC changes.
Google Business Profile rating improved from 3.1 ★ to 4.0 ★ in 6 months. Daily patient volume increased from 118 to 134 (13.6%). At the clinic’s estimated $42 average OHIP billing per visit and 310 operating days, the volume increase represented $83,000 in additional annual OHIP billings. Payback period on the $38,000 renovation: less than 6 months.
Case Study 2: Vaughan Multi-Physician Practice — Full Renovation ROI
A 4-physician Family Health Organization practice in Vaughan completed a full 3,200 sq ft renovation at a total cost of $387,000. The scope included: reconfigured exam rooms (from 8 small non-compliant rooms to 6 AODA-compliant rooms with proper turning radius), centralized nurse station, new reception and waiting area with accessible lowered counter, updated HVAC for infection control, and full AODA compliance scope.
The practice secured a landlord TI allowance of $52/sq ft ($166,400), reducing net renovation cost to $220,600. Patient roster additions in the 24 months post-renovation: 340 newly enrolled patients. At an average capitation weight of $220/patient/year, the new enrollments generate $74,800 in annual recurring revenue. Staff turnover dropped from 4 annual departures to 1, saving an estimated $36,000 annually. Combined annual benefit: $110,800. Payback on net renovation cost ($220,600): 24 months.
Case Study 3: Newmarket Specialist Clinic — Compliance-Focused ROI
A Newmarket dermatology practice received an AODA compliance audit ahead of a planned practice sale. The audit identified 9 non-conformances estimated to trigger a $90,000–$140,000 purchase price discount if left unremediated. The practice invested $74,000 in targeted compliance renovation: accessible entrance (new automatic door, ramp extension), accessible washroom retrofit, reception counter modification, and exam room layout adjustment for wheelchair turning radius.
The practice sold 14 months later. The purchasing physician’s offer reflected a $0 compliance discount — compared to the $110,000 discount that had been offered by a different buyer before the renovation. Net return on $74,000 investment: $110,000 at sale, plus $36,000 in additional OHIP billings during the 14 months of improved operational efficiency post-renovation. Total return: approximately $146,000 on a $74,000 investment within 14 months.
The 5-Year Renovation Cycle: Planning Your Investment Roadmap
The most capital-efficient approach to medical office renovation is not a single large project every 15–20 years. It is a structured 5-year cycle that maintains facility quality continuously, spreads capital investment, and keeps compliance current with evolving AODA and CPSO standards.
Year 1–2: Cosmetic and Compliance Baseline
Address visible patient experience factors (flooring, paint, lighting, seating) and complete an AODA compliance gap assessment. Resolve any compliance findings. Investment: $20,000–$60,000. Annual maintenance budget: $8,000–$15,000 for ongoing repairs and updates.
Year 2–3: Operational Efficiency Improvements
Add exam room capacity if volume supports it, reconfigure nurse station and workflow bottlenecks, upgrade HVAC for infection control where needed. Investment: $45,000–$120,000 depending on scope.
Year 3–4: Technology Integration
Electronic check-in, updated EMR workstation infrastructure, telehealth room designation, patient-facing digital displays in waiting areas. Investment: $15,000–$40,000.
Year 5: Full Assessment and Strategic Renovation Planning
Commission a comprehensive facility assessment against current CVO/CPSO standards, current AODA DOPS requirements, and practice strategic plan. Plan the next 5-year cycle. If a complete renovation is warranted, initiate design and permit process with an 18-month implementation horizon. This structured approach keeps annual capital requirements manageable ($20,000–$80,000/year on average) and prevents the accumulation of deferred maintenance that drives the large, disruptive, high-cost single-event renovations that most clinic owners find overwhelming.
Tax and Financing Considerations for Ontario Clinic Renovations
Understanding the tax treatment of renovation investment is part of accurate ROI calculation. Key considerations for Ontario medical clinic owners:
Leasehold improvements: CRA classifies leasehold improvements as Class 13 capital assets, amortized over the lesser of the lease term or 20 years, at 20% per year (declining balance). A $200,000 renovation on a 10-year lease generates $40,000 in CCA deductions in Year 1, $32,000 in Year 2, etc. — reducing taxable income in each year and improving after-tax ROI.
Equipment purchases: Medical equipment (exam tables, sterilization equipment, diagnostic tools) purchased as part of a renovation is typically Class 8 (20% CCA) or Class 14.1 — deductible separately from the building renovation.
GST/HST: Medical services are GST/HST exempt in Canada, which means medical clinic operators generally cannot claim Input Tax Credits on renovation costs (HST paid on renovation is a real cost, not recoverable). However, if the clinic has any non-exempt revenue streams (cosmetic procedures, dispensary sales, etc.), partial ITC recovery may be available — consult a healthcare-specialist accountant.
Financing options: Major chartered banks have healthcare lending divisions that offer specialized renovation financing for medical practices at rates 0.5–1.5% below standard commercial rates. Terms of 5–10 years are typical for clinic renovation financing. The Royal Bank Healthcare practice financing, TD Health Practice Finance, and BDC’s healthcare lending programs are the primary options for Ontario clinic owners. Equipment-specific purchases may qualify for lower-rate equipment financing separate from the renovation loan.
Frequently Asked Questions: Medical Office Renovation ROI
How long does it take for a medical office renovation to pay for itself?
Payback period varies significantly by renovation scope, practice type, and how well the renovation addresses the practice’s specific ROI drivers. Cosmetic refreshes ($20,000–$45,000) typically achieve payback within 18–36 months through improved patient acquisition and staff satisfaction. Full fit-out renovations ($175,000–$400,000) typically achieve payback within 4–7 years when all five ROI drivers are considered — patient volume, staff retention, regulatory risk avoidance, property value, and practice sale value. Compliance-focused renovations often achieve payback faster than their scope suggests, because the risk avoidance value (HRTO exposure, AODA penalties, sale price discounts) can be quantified independently of any operational improvement. The most accurate payback calculation considers: (a) net renovation cost after landlord TI allowance; (b) annual revenue increase from patient volume gains; (c) annual cost savings from staff retention improvement; (d) annualized legal risk reduction; and (e) improvement to practice sale value discounted over expected ownership horizon.
How do I measure the ROI of my clinic renovation?
A structured pre/post measurement approach gives you the clearest data. Before your renovation begins, document and baseline four metrics: average monthly OHIP billings (or patient visit volume), monthly new patient requests (or roster addition rate), annual staff turnover count, and Google Business Profile rating with review sentiment analysis. After renovation, track the same metrics monthly for 24 months. The difference in each metric — expressed in dollar value — is your measurable ROI. Avoid attributing all practice growth post-renovation to the renovation itself; external factors (population growth, competitor clinic closings, physician marketing activity) may contribute. A reasonable attribution methodology: assume 50–70% of measurable improvement in the 24 months post-renovation is attributable to the renovation, with the remainder to other factors. Even this conservative attribution consistently supports positive ROI for well-executed clinic renovations in the GTA market.
Should I renovate before or after adding a new physician to the practice?
In almost every case, renovate before adding the physician. The reason is straightforward: a new physician joining an outdated clinic facility will either accept the existing conditions (and begin advocating for renovation immediately, creating internal tension) or decline the opportunity after visiting the facility. Renovating first — specifically adding exam room capacity, updating the nurse station, and improving patient flow — signals to prospective associate physicians that the practice is professionally managed and invested in working conditions. It also ensures the new physician can function at full clinical capacity from day one, rather than sharing rooms or operating in compromised workflow conditions. The financial case is equally clear: the revenue contribution of a full-capacity associate physician ($200,000–$350,000 in annual OHIP billings) begins accumulating the day they start seeing patients, while the renovation cost is amortized over years. Sequencing matters: invest in capacity before adding the capacity user.
What financing options exist for Ontario medical clinic renovations?
Ontario medical clinic owners have several financing pathways, each with different terms and eligibility criteria. Major chartered bank healthcare divisions (RBC, TD, Scotiabank) offer practice renovation loans at prime + 0.5–1.5% for established practices with 3+ years of billing history, with terms of 5–10 years and amortization periods up to 15 years for larger projects. The Business Development Bank of Canada (BDC) offers healthcare-specific term loans with fixed rates and flexible repayment schedules — particularly useful for practices that have irregular revenue cycles. Equipment vendors for medical examination equipment, sterilization systems, and diagnostic tools often offer direct financing at competitive rates as part of procurement packages. Provincial grant programs: while direct renovation grants for private medical practices are limited, practices that include accessibility improvements may qualify for Ontario government accessibility grants under the Enabling Accessibility Fund — check eligibility at the Employment and Social Development Canada website. Landlord TI allowances, as noted elsewhere in this guide, represent a significant potential offset to renovation cost that is available through negotiation rather than application — and is often not pursued by clinic owners who don’t know to ask for it.
What is the best time of year to renovate a medical clinic in Ontario?
The optimal timing for a clinic renovation in Ontario balances three factors: contractor availability, patient volume patterns, and HVAC commissioning requirements. Contractor availability is highest from January through April — GTA construction demand peaks in spring and summer as outdoor projects resume, making winter the window for most favourable pricing (5–15% savings are commonly reported for full-closure renovations completed between January and March). Patient volume in most Ontario family medicine practices peaks in fall and winter (respiratory illness season) and troughs in July–August when both patients and staff take vacation. A renovation timed to be substantially complete before September avoids the peak demand period and allows the new facility to capture the fall patient acquisition window. HVAC commissioning timing: HVAC systems should be commissioned and balanced during a season where outdoor conditions allow the system to be tested across a reasonable temperature range — spring (April–May) or fall (September–October) are optimal for commissioning verification. Plan your construction schedule to reach mechanical completion by mid-April or mid-September to allow proper commissioning time before summer heat or winter cold stress-tests the system.
Does renovating a medical office affect its CPSO compliance status?
Yes — and in two directions. A renovation that brings a facility into full compliance with CPSO office practice standards, AODA requirements, and current infection control guidelines can directly improve a practice’s standing in CPSO quality assurance assessments. The CPSO’s Physician Practice Enhancement Program evaluates physical facility components as part of broader practice quality assessment. Conversely, a renovation that disrupts facility systems — temporarily removing infection control infrastructure, creating construction dust in clinical areas, or disabling accessibility accommodations — can create temporary compliance concerns if the practice attempts to operate during construction without proper safeguards. The specific risk: operating an open clinical environment adjacent to active construction without proper dust control and air separation constitutes an infection control risk that CPSO could cite if a complaint arose during the construction period. Properly managed, phased renovations with physical separation between construction and clinical zones — and temporary supplemental air filtration in operating clinical areas — mitigate this risk. Your renovation contractor should have documented infection prevention and control (IPAC) procedures for active construction in occupied healthcare facilities — ask for them before signing any contract.
How much does not renovating actually cost?
This is the question most clinic owners never ask — and the most important one in the renovation ROI analysis. The cost of not renovating includes: incremental patient attrition (estimated 1–3% annually for practices with below-market facility quality in competitive GTA markets, compounding over years); staff turnover premium (outdated facilities consistently correlate with higher staff turnover, adding $8,000–$25,000 per departure); accumulating deferred maintenance cost (mechanical systems, flooring, and surfaces in poor repair cost more to replace urgently than to maintain proactively — emergency HVAC replacement in a clinic mid-winter runs 40–60% more than planned replacement); AODA exposure accumulation (the legal risk of inaccessible facilities grows, not shrinks, over time as enforcement becomes more active); and practice sale discount (every year a practice with a deferred renovation is held is a year that potential sale price discount risk accumulates). When these costs are annualized and modelled over a 5-year period, the “cost of not renovating” for a typical GTA medical practice in outdated facilities frequently exceeds $40,000–$90,000 per year — often more than the annualized cost of the renovation itself.
What should I look for in a medical renovation contractor for an ROI-focused project?
An ROI-focused renovation requires a contractor who understands not just construction but healthcare facility compliance and operational impact. The five contractor evaluation criteria most relevant to ROI outcomes: First, documented experience with Ontario medical clinic renovation specifically — not just healthcare broadly. Ask for three GTA medical clinic references completed in the past three years, contact them, and ask specifically about post-renovation operational improvements and compliance outcomes. Second, knowledge of current CPSO, AODA, and OBC requirements — a contractor who cannot articulate what AODA Design of Public Spaces Standards require for accessible medical reception counters does not have current healthcare regulatory knowledge. Third, IPAC (infection prevention and control) construction protocols — the contractor should have documented procedures for constructing in or adjacent to occupied clinical space, including dust barriers, air pressure management, and construction traffic separation from patient areas. Fourth, a network of qualified trade contractors — mechanical (HVAC), electrical, and plumbing trade partners who have specifically worked in healthcare environments and understand the more demanding specifications that clinical spaces require. Fifth, project management approach to minimizing clinical downtime — the contractor should be able to present a phasing strategy that explicitly maps construction activities against your clinical schedule, identifying which phases require full closure and which can proceed with partial operation.
How to Calculate Your Specific Clinic Renovation ROI
The ROI frameworks in this guide are based on documented Ontario clinic outcomes — but your practice’s specific ROI calculation depends on your unique variables. Here is a step-by-step approach to producing a defensible, practice-specific ROI estimate before you commit to a renovation budget.
Step 1: Quantify Your Current Leakage
Before you can calculate renovation ROI, you need to estimate how much revenue the current facility state is costing you. Pull three data points: your Google Business Profile rating (and the percentage of negative reviews that cite facility quality — you can sort reviews by keyword in Google Business Profile manager); your new patient request rate over the past 12 months compared to 3 years ago; and your staff turnover rate over the past 3 years. For each metric that shows deterioration, estimate the revenue or cost impact using the benchmarks in this guide. A 0.5-star drop in Google Business Profile rating correlates with approximately 10–15% reduced new patient inquiry rate in GTA healthcare practices — a quantifiable starting point for your loss-side calculation.
Step 2: Model the Revenue Upside
Based on the renovation scope you’re considering, estimate revenue recovery using your practice’s actual billing rates. For OHIP-billing family medicine: each 1 additional patient per day, 310 days per year, at your practice’s average fee per visit, generates a specific annual revenue number. Calculate it with your actual numbers. For capitated practices: each additional enrolled patient at your blended capitation rate (typically $180–$280 for a standard adult patient mix) generates recurring annual revenue. Model 5 years of that recurring revenue, discounted at 5% for conservatism, to get the net present value of new patient acquisition. This present-value approach often reveals that the revenue upside of improved new patient acquisition is dramatically larger than the renovation cost when properly modelled over a 5-year horizon.
Step 3: Add the Risk Avoidance Value
Consult with your healthcare lawyer or practice management advisor on your specific AODA compliance gap. Ask for a rough estimate of HRTO exposure based on the specific non-conformances in your facility. Even a ballpark range ($50,000–$150,000 typical exposure for a moderate AODA compliance gap in a medical practice) can be included in your ROI model as a risk-adjusted value. If your probability-weighted exposure over 5 years is $30,000, that $30,000 belongs in your renovation ROI calculation as a benefit of compliant renovation — because the renovation eliminates that exposure.
Step 4: Get the Landlord TI Number First
Before finalizing your renovation budget, talk to your landlord about a tenant improvement allowance. Many Ontario clinic owners skip this step and fund their renovation entirely from practice cash flow or loans — leaving $25,000–$85,000 of landlord contribution on the table. The TI conversation is a negotiation: your leverage is the fact that you’re a high-quality, long-term medical tenant committing to a multi-year lease renewal. Start by confirming your intent to renew the lease as part of the renovation discussion; most landlords will then engage on TI as part of the lease renewal terms. The TI allowance you secure directly reduces your net renovation cost and improves every ROI metric in your model.
Step 5: Build Your Break-Even Table
Compile your numbers into a simple break-even table: renovation cost (net of TI allowance) in one column; annual benefit (revenue gain + cost savings + annualized risk reduction) in the other. Divide net renovation cost by annual benefit to get payback years. For most well-planned GTA medical clinic renovations, this calculation yields a payback period of 3–6 years — well within the economic life of the renovation and the expected lease term. If your calculation shows a payback period exceeding 8 years, it typically signals either that the renovation scope is broader than your current practice requires, or that your revenue leakage from the current facility is lower than average — meaning the renovation is still valuable but primarily as a compliance and practice-value investment rather than a near-term revenue driver.
Renovation ROI by Practice Specialty
ROI mechanics vary by practice specialty because the patient decision-making process, OHIP billing structure, and competition landscape differ across medical disciplines. The following profiles summarize the dominant ROI drivers by specialty type in the Ontario market.
| Specialty | Primary ROI Driver | Secondary ROI Driver | Typical Payback Period | Notes |
|---|---|---|---|---|
| Family Medicine / GP | Patient acquisition (capitation) | Staff retention | 3–6 years | Recurring capitation revenue compounds over years |
| Walk-In Clinic | Patient volume (fee-for-service) | Online review improvement | 1–3 years | Highest volume sensitivity to facility quality |
| Physiotherapy / Rehab | Patient experience + referral | Staff productivity | 3–5 years | Referral relationships affected by facility quality |
| Dental | New patient acquisition | Treatment acceptance rate | 2–4 years | Premium facility drives higher case acceptance |
| Dermatology | Practice sale value | Patient acquisition | 2–4 years (or immediate at sale) | High practice sale premium for modern facilities |
| Pharmacy | OCP compliance + foot traffic | Dispensing volume | 3–5 years | Regulatory compliance is primary driver |
Walk-in clinics show the fastest payback because their revenue model is entirely fee-for-service — every additional patient seen translates directly to additional OHIP billings with no enrollment lag. A walk-in clinic seeing 100 patients per day at an average $38 OHIP billing per visit generates approximately $1.4M in annual billings; a 10% volume improvement from renovation-driven Google review improvement represents $140,000 in additional annual billings — recovering a $200,000 renovation in 17 months.
Your 30-Day Action Plan: Starting Your Renovation ROI Process
The clinic owners who achieve the strongest renovation ROI are the ones who begin the planning process early — not the ones who wait until the carpet is visibly worn or the CVO inspector has been to the door. Here is a concrete 30-day action plan to begin your renovation ROI process without committing to any major expense.
- Days 1–5: Document your baseline. Pull 12 months of OHIP billing data or patient visit volume. Export your Google Business Profile review history. Calculate your staff turnover count for the past 3 years. These three data sets are the inputs to your ROI model and cost nothing to gather.
- Days 5–10: Commission an AODA compliance audit. A healthcare-experienced architect or accessibility consultant can complete a walk-through audit of your facility against current AODA Design of Public Spaces Standards in 2–3 hours. Cost: $500–$1,500. Output: a documented list of non-conformances and estimated remediation costs. This audit is the single most valuable $1,000 a clinic owner can spend before planning a renovation.
- Days 10–15: Talk to your landlord. Request a meeting to discuss lease renewal and tenant improvement allowance. You do not need to have renovation plans to start this conversation — only an intent to renew and an interest in understanding what TI support the landlord would consider. The response will tell you whether TI is available and in what range, shaping your renovation budget ceiling significantly.
- Days 15–25: Get three preliminary renovation estimates. Contact three contractors with documented Ontario medical clinic renovation experience. Share the AODA audit results and any specific operational needs (additional exam room, nurse station reconfiguration, etc.) and ask for a ballpark cost range — not a detailed quote yet. This gives you a realistic cost range to model against your ROI calculation.
- Days 25–30: Build your ROI model. Using the steps outlined in this guide, compile your leakage estimate, revenue upside model, risk avoidance value, net renovation cost (after TI), and annual benefit figure. Calculate your payback period. Present this analysis to your accountant or financial advisor before committing to any scope. A renovation that pencils out on paper with your specific practice numbers, at your specific TI-adjusted net cost, is a renovation worth proceeding with.
The clinics in the GTA that are growing their patient rosters, retaining their staff, and commanding premium practice sale prices are not operating in superior facilities by accident. They made a deliberate decision to treat renovation as investment rather than expense — and then they did the math to back it up. Dr. Nguyen wishes she’d done the math in 2019. You have the tools to do it now.
Written by the RenoEthics construction team — specialists in Ontario medical clinic renovation and healthcare facility compliance. Last updated March 2026. RenoEthics has completed medical office renovations across Richmond Hill, Markham, Vaughan, Newmarket, Aurora, Toronto, and the broader GTA. Schedule a facility assessment or request a renovation quote today.